| Outbreak: Berry Stand Strawberries | |
|---|---|
| Product: Strawberries | Investigation Start Date: 08/03/2011 |
| Location: Clackamas, Multnomah, Washington, Clatsop, & Yamhill Counties, Oregon | Etiology: E. coli (STEC) O157:H7 |
| Earliest known case onset date: 07/01/2011 | Latest case onset date: 07/29/2011 |
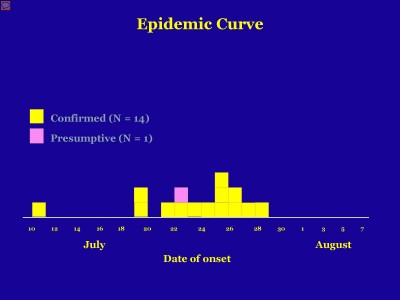
| Confirmed / Presumptive Case Counts: 14 / 1 | Positive Samples (Food / Environmental): 4 / 100 |
| Hospitalizations: 6 | Deaths: 2 |
This investigation implicated a novel vehicle—strawberries—as the cause of an outbreak of E. coli O157 infections. An association with locally produced strawberries quickly became apparent as cases were interviewed; but the fact that almost all had purchased them at roadside stands and farmer’s markets led to concern about potential confounding of some overlooked item sold at similar venues. The concern was laid to rest by visits to the stands, a case-control study, and traceback of the strawberries to a single Oregon farmer. Learning how the strawberries became contaminated was the fruit of field work: epidemiologists investigated the strawberry fields and found them heavily contaminated with deer feces, with a herd of deer seen grazing in the area. Culture of 50 environmental samples that contained visible deer pellets yielded E. coli O157 in 10 (20%), with PFGE patterns matching those of the cases.
This outbreak once again confirmed deer as key reservoirs for the pathogen. Interestingly, an additional PFGE-matched case was identified months later; the case hadn’t eaten the commercial strawberries but lived in the area where they were grown. Culture of a sample from this case household’s vacuum cleaning bag yielded a PFGE-matching strain of E. coli O157:H7, a testimony to the pathogen’s ability to survive for prolonged periods when dried.
The following is the abstract from the published article found here. Editorial commentary can be found here.
BACKGROUND:
An outbreak of Escherichia coli O157:H7 was identified in Oregon through an increase in Shiga toxin-producing E. coli cases with an indistinguishable, novel pulsed-field gel electrophoresis (PFGE) subtyping pattern.
METHODS:
We defined confirmed cases as persons from whom E. coli O157:H7 with the outbreak PFGE pattern was cultured during July–August 2011, and presumptive cases as persons having a household relationship with a case testing positive for E. coli O157:H7 and coincident diarrheal illness. We conducted an investigation that included structured hypothesis-generating interviews, a matched case-control study, and environmental and traceback investigations.
RESULTS:
We identified 15 cases. Six cases were hospitalized, including 4 with hemolytic uremic syndrome (HUS). Two cases with HUS died. Illness was significantly associated with strawberry consumption from roadside stands or farmers’ markets (matched odds ratio, 19.6; 95% confidence interval, 2.9–∞). A single farm was identified as the source of contaminated strawberries. Ten of 111 (9%) initial environmental samples from farm A were positive for E. coli O157:H7. All samples testing positive for E. coli O157:H7 contained deer feces, and 5 tested farm fields had ≥ 1 sample positive with the outbreak PFGE pattern.
CONCLUSIONS:
The investigation identified fresh strawberries as a novel vehicle for E. coli O157:H7 infection, implicated deer feces as the source of contamination, and highlights problems concerning produce contamination by wildlife and regulatory exemptions for locally grown produce. A comprehensive hypothesis-generating questionnaire enabled rapid identification of the implicated product. Good agricultural practices are key barriers to wildlife fecal contamination of produce.